Clubfoot repair surgery is performed to improve the position and function of a foot and ankle affected by this birth condition. A podiatrist can determine if surgery is needed based on the severity of the deformity and prior treatment. During the clubfoot repair surgery, adjustments are made to the tendons to help the foot move into a more natural position. This may include lengthening the Achilles tendon. In some cases, small bone corrections may be required to support proper alignment. After surgery, a cast is placed on the baby’s foot to protect it and assist with healing. The cast is typically worn for several weeks and may need to be changed a few times. As the foot heals, follow-up care helps ensure the best possible outcome. While some stiffness may remain, surgery can greatly improve mobility and allow for an active lifestyle. If your child was born with clubfoot, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
Congenital foot problems require immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Graff Foot, Ankle and Wound Care. Our doctors can provide the care you need to keep you pain-free and on your feet.
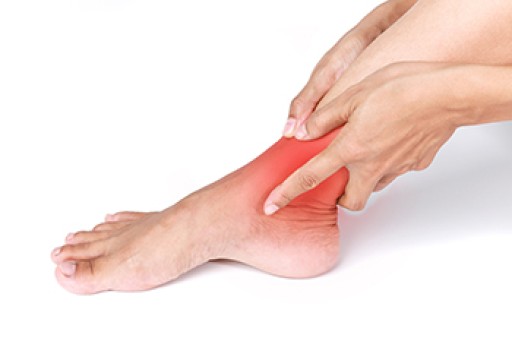
Congenital foot problems are deformities affecting the feet, toes, and/or ankles that children are born with. Some of these conditions have a genetic cause while others just happen. Some specific foot ailments that children may be born with include clubfeet, polydactyly/macrodactyly, and cleft foot. There are several other foot anomalies that can occur congenitally. What all of these conditions have in common is that a child may experience difficulty walking or performing everyday activities, as well as trouble finding footwear that fits their foot deformity. Some of these conditions are more serious than others. Consulting with a podiatrist as early as possible will help in properly diagnosing a child’s foot condition while getting the necessary treatment underway.
What are Causes of Congenital Foot Problem?
A congenital foot problem is one that happens to a child at birth. These conditions can be caused by a genetic predisposition, developmental or positional abnormalities during gestation, or with no known cause.
What are Symptoms of Congenital Foot Problems?
Symptoms vary by the congenital condition. Symptoms may consist of the following:
- Clubfoot, where tendons are shortened, bones are shaped differently, and the Achilles tendon is tight, causing the foot to point in and down. It is also possible for the soles of the feet to face each other.
- Polydactyly, which usually consists of a nubbin or small lump of tissue without a bone, a toe that is partially formed but has no joints, or an extra toe.
- Vertical talus, where the talus bone forms in the wrong position causing other bones in the foot to line up improperly, the front of the foot to point up, and the bottom of the foot to stiffen, with no arch, and to curve out.
- Tarsal coalition, when there is an abnormal connection of two or more bones in the foot leading to severe, rigid flatfoot.
- Cleft foot, where there are missing toes, a V-shaped cleft, and other anatomical differences.
- Macrodactyly, when the toes are abnormally large due to overgrowth of the underlying bone or soft tissue.
Treatment and Prevention
While there is nothing one can do to prevent congenital foot problems, raising awareness and receiving neonatal screenings are important. Early detection by taking your child to a podiatrist leads to the best outcome possible.
If you have any questions please feel free to contact our offices located in Plano, Dallas, Prosper, Allen, Irving, Garland, Frisco, and Coppell, TX . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.