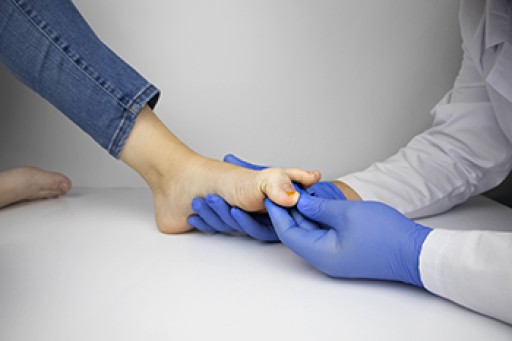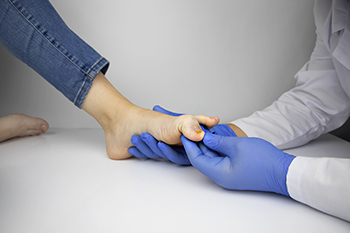
Dealing with stubborn fungal toenails? Surgical toenail removal might be the solution. This procedure is typically done in a podiatrist's office under local anesthesia to ensure comfort. The toenail removal process involves loosening the skin around the toenail and removing either the entire nail or just the affected portion, depending on the severity of the infection. To prevent regrowth and future fungal toenail infections, the nail matrix can be destroyed using a chemical solution after removal. Post-surgery, proper wound care includes gentle washing with clean water and avoiding harsh substances like hydrogen peroxide or alcohol. Healing usually takes a few weeks, with toenails growing back within a year to 18 months. Surgical toenail removal is reserved for cases where a significant portion of the nail is diseased or causing severe pain. If fungal toenails are impacting your life, it is suggested that you make an appointment with a podiatrist to explore treatment options, including surgical intervention if necessary.
For more information about treatment, contact one of our podiatrists of Graff Foot, Ankle and Wound Care. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our offices located in Plano, Dallas, Prosper, Allen, Irving, Garland, Frisco, and Coppell, TX . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.